Probability of Malignancy in SPN: Bayesian Analysis
A common radiographic problem is the evaluation of the patient with a solitary pulmonary nodule (SPN). Ninety percent of SPN's are due to 5 causes: lung cancer, granuloma, solitary metastasis, hamartoma, and carcinoid tumors. Because the frequency of malignancy is high, accurate evaluation is important. Both clinical and radiographic factors are important in this determination. It can be difficult to subjectively combine all of the radiographic and clinical findings in a given patient and arrive at a diagnosis. Often, important factors such as smoking history, are either ignored or overemphasized. The main objective of Bayesian analysis is to use all of the clinical and radiographic characteristics to derive a quantitative estimate of the probability that a SPN is malignant.
The following form can be used to derive the probability of malignancy and is based on data provided in the first reference.
The prior odds of malignancy can be subjectively estimated or based on the prevalence of malignancy in your patient population with solitary pulmonary nodules. The latter will vary by geographic location (due to histoplasmosis) or vary by referral pattern (tertiary care hospital vs clinic).
Probability of Malignancy in SPN: Logistic Regression
Compare the above result to this method derived from multivariate logistic regression in 629 patients (65% benign, 23% malignant, 12% indeterminate). The equation is based on 3 clinical and 3 radiographic variables.
Probability of Malignancy = ex(1 + ex)
where x = -6.8272 + (0.0391 * Age) + (0.7917 * Cigarettes) + (1.3388 * Cancer) + (0.1274 * Diameter) + (1.0407 * Spiculation) + (0.7838 * Upper).
Note: this equation is not applicable to patients with a diagnosis of cancer that has been made within the previous 5 years or to patients with previous lung cancer.
Likelihood Ratios:
Likelihood ratios are intuitive measures of the diagnostic information provided by a test result or clinical finding. The likelihood ratio varies from zero to infinity, depending on the degree of malignancy or benignity of the test result. A test strongly suggestive of malignancy has a likelihood ratio much greater than one, a test that suggests benignity has a likelihood ratio close to zero, and a test that contains no diagnostic information has a likelihood ratio of one. In the odds-likelihood ratio form of Bayes theorem, the odds that a SPN is malignant is the product of the likelihood ratios favoring malignancy for each nodule or patient characteristic multiplied by the prior odds of malignancy.
Equations:
Bayes Theorem:
- Posterior odds = prior odds x likelihood ratios
Likelihood Ratios:
- Prob in subjects with malignancy / Prob in subjects without malignancy
- Sensitivity / (1 - Specificity)
- True positive fraction / False positive fraction
Probability:
- Probability = Odds / (Odds + 1)
- Odds = Prob / (1 - Prob)
Note the following: A likelihood ratio of 1 does not change prior and post odds (or probabilities). As the likelihood ratio approaches 0 the chances that a disease exists is nil. Once the likelihood ratio exceeds 10, the probability that the disease exists is extremely high (ie. the finding is pathognomonic). Changing the sensitivity and specificity changes the likelihood ratio.
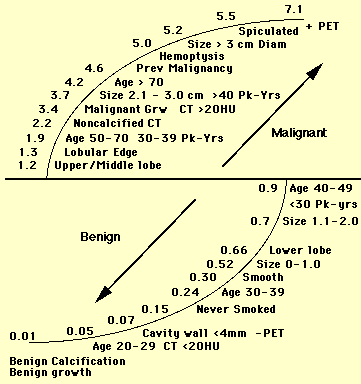
Any characteristic above 1 increases the likelihood of malignancy. Some such as location are weak, others are very strong (spiculated edge). Conversely, characteristics less than 1 decrease the likelihood of malignancy. Again the strength can be quantitated.
| References |
|
Gurney JW. Determining the likelihood of malignancy in solitary pulmonary nodules with Bayesian analysis. Part I. Theory. Radiology 1993; 186:405-413. [Related Records] Gurney JW, Lyddon DM, McKay JA. Determining the likelihood of malignancy in solitary pulmonary nodules with Bayesian analysis. Part II. Application. Radiology 1993; 186:415-422. [Related Records] Black WC, Armstrong P. Communicating the significance of radiologic test results: the likelihood ratio. AJR 1986; 147:1313-1318. [Related Records] Swensen SJ, Silverstein MD, Ilstrup DM, Schleck CD, Edell ES. The probability of malignancy in solitary pulmonary nodules. Application to small radiologically indeterminate nodules. Arch Intern Med 1997; 157:849-855. [Related Records] Dewan NA, Shehan CJ, Reeb SD, et al. Likelihood of malignancy in a solitary pulmonary nodule: comparison of Bayesian analysis and results of FDG-PET scan. Chest 1997; 112:416-422. [Related Records] Disclaimer: Information provided is not intended to be medical or technical advice. The information given at this site is for educational purposes only and is not sufficient for medical decisions. I disclaim any liability for the acts of any physicians or any other individual who receives any information on any medical procedure through this web site. I accept no legal responsibility for any injury and/or damage to persons or property from any of the suggestions or material discussed herein. |
